Protti A, Chiumello D, Cressoni M, Carlesso E, Mietto C, Berto V, et al. Prone position-induced improvement in gas exchange does not predict improved survival in the acute respiratory distress syndrome. Diminishing efficacy of prone positioning with late application in evolving lung injury. Xin Y, Martin K, Morais CCA, Delvecchio P, Gerard SE, Hamedani H, et al. Prone positioning and survival in mechanically ventilated patients with coronavirus disease 2019-related respiratory failure. Mathews KS, Soh H, Shaefi S, Wang W, Bose S, Coca S, et al. Prone positioning in severe acute respiratory distress syndrome. Guérin C, Reignier J, Richard J-C, Beuret P, Gacouin A, Boulain T, et al. An Official American Thoracic Society/European Society of Intensive Care Medicine/Society of Critical Care Medicine clinical practice guideline: mechanical ventilation in adult patients with acute respiratory distress syndrome. 2010 76(6):448–54.įan E, Del Sorbo L, Goligher EC, Hodgson CL, Munshi L, Walkey AJ, et al. Prone positioning improves survival in severe ARDS: a pathophysiologic review and individual patient meta-analysis. Gattinoni L, Carlesso E, Taccone P, Polli F, Guerin C, Mancebo J. Beneficial hemodynamic effects of prone positioning in patients with acute respiratory distress syndrome. Jozwiak M, Teboul JL, Anguel N, Persichini R, Silva S, Chemla D, et al. Paradoxical effect of chest wall compression on respiratory system compliance: a multicenter case series of patients with ARDS, with multimodal assessment. 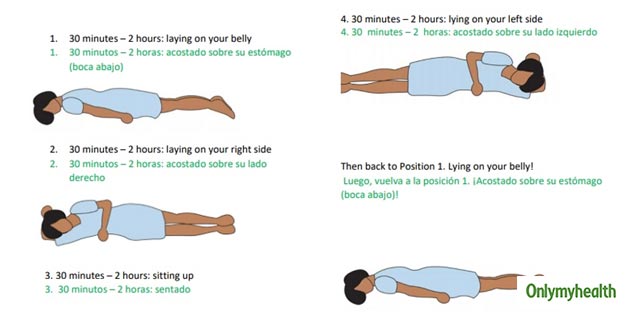
Rezoagli E, Bastia L, Grassi A, Chieregato A, Langer T, Grasselli G, et al. Effect of body position and inclination in supine and prone position on respiratory mechanics in acute respiratory distress syndrome. Influence of PEEP titration on the effects of pronation in ARDS: a comprehensive experimental study. Scaramuzzo G, Ball L, Pino F, Ricci L, Larsson A, Guérin C, et al. Body position changes redistribute lung computed-tomographic density in patients with acute respiratory failure. Gattinoni L, Pelosi P, Vitale G, Pesenti A, D’Andrea L, Mascheroni D. Clinical characteristics and day-90 outcomes of 4244 critically ill adults with COVID-19: a prospective cohort study. Epidemiology, patterns of care, and mortality for patients with acute respiratory distress syndrome in intensive care units in 50 countries. 
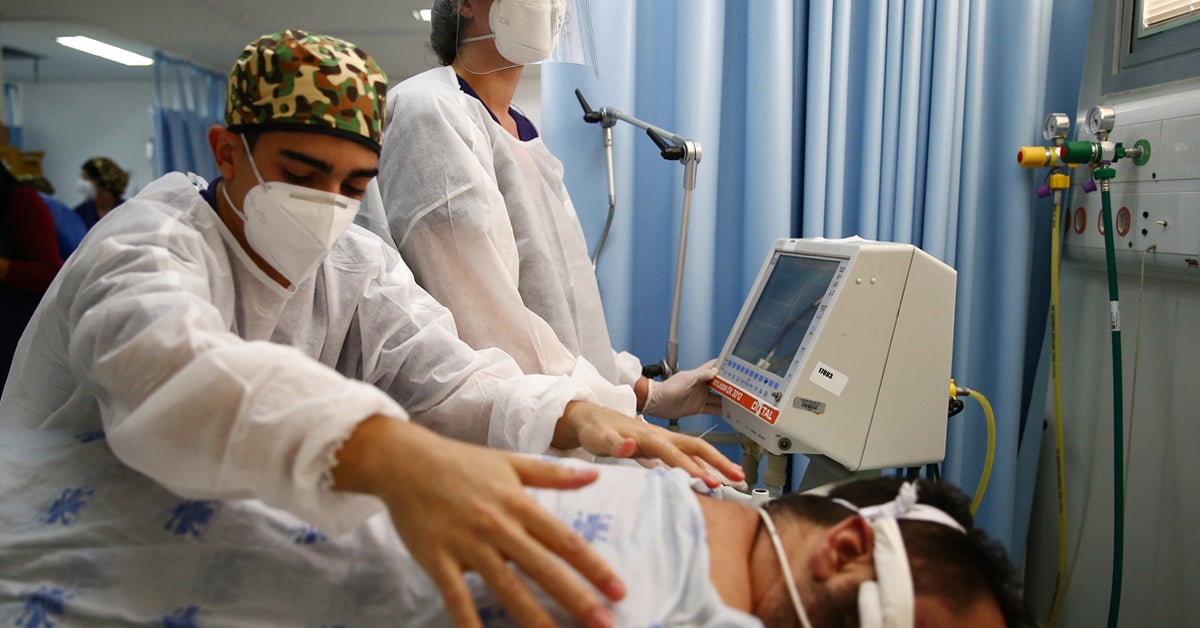
2018 44(1):22–37.īellani G, Laffey JG, Pham T, Fan E, Brochard L, Esteban A, et al. A prospective international observational prevalence study on prone positioning of ARDS patients: the APRONET (ARDS Prone Position Network) study. Guerin C, Beuret P, Constantin JM, Bellani G, Garcia-Olivares P, Roca O, et al. The recent observational studies on COVID-19-related ARDS suggest the beneficial effect of proning on outcome with an early application and in responders in terms of oxygenation of the proning cycles. There are three main physiological benefits in proning an ARDS patient: to get better oxygenation, to get a better control of lung stress and strain imposed by the mechanical ventilation over the ones due to the ARDS per se and to stabilize and even improve hemodynamics. This chapter will cover rationale, timing, some practical issues, and clinical results, including those observed during the COVID-19 pandemic, of the use of prone position. Interestingly, this changing in rate of use of proning has been observed for the same level of evidence. Its rate of use increased from 10 to 30% in the classic acute respiratory distress syndrome (ARDS) before the SARS-Cov-2 pandemic to more than 70% in the COVID-19-related ARDS. Prone position has been used for almost 50 years from now.
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
